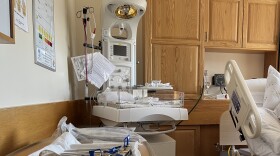
Before COVID-19 struck last year, the 18-bed ICU at Portsmouth Regional Hospital was already a busy place, full of post-surgery patients and emergency admissions: people suffering from heart attacks, strokes and pneumonia.
There, Dr. Dawn Barclay and her staff put their decades of experience, and centuries of medical knowledge, to use every day to guide treatment.
But in this pandemic, there’s just no precedent to turn to.
“COVID is different,” Barclay said. “You see young healthy people really with little to no comorbidities who...come in with a thromboembolic complication. What that means is they have blood clots, and it takes their life. Bam. Gone.”
Those deaths, all of which Barclay calls preventable, piled up in New Hampshire this winter. Fueled by holiday gatherings, and a continued reluctance by some to follow public health guidelines, more than 530 residents died in December and January alone, nearly half of the total COVID-19 related deaths recorded in the state since the pandemic began. On any given day through most of December and January, New Hampshire hospitals were treating between 200 and 300 people for COVID-19 — far more than were reported during any earlier wave of the pandemic, according to the available data.
Loading...
While new cases, hospitalizations and deaths from COVID-19 have leveled off in recent days, many New Hampshire hospitals are still grappling with the stress and deep sense of loss that came during the pandemic’s darkest days.
“It feels senseless to me. It really does. And it can at times bring you really down, because you feel powerless,” Barclay said.
That feeling of powerlessness lingers across New Hampshire’s entire health care system. At Lakes Region General Hospital, the peak of the latest surge in early January left the small hospital treating 13 COVID-positive patients simultaneously.
The number of inpatients has declined since then — a result of discharges, as well as patient deaths.
“I feel like this is a new evolving disease process; what we knew in March was very little and what we know, we try everything we can,” said Jamie LaRoche, a nurse practitioner at LRG. “I think everyone is ready and willing to pitch in to do whatever they can, and still sometimes that’s not enough, and I think that’s really hard for a lot of our clinical staff and providers to have to process through.”
Last spring, health workers were treated as heroes, with people banging pots and pans, donating food to hospitals, and children making signs. Cass Walker, a vice president at LRG, said some of that public outpouring has inevitably faded.
“Because the pandemic has gone on for almost a year now, there is less of that,” said Walker. “Our whole society is exhausted.”
Loading...
Along with mental and physical burnout, there’s also the ongoing financial challenge facing New Hampshire hospitals. COVID-19 forced the cancellation or delay of non-essential procedures, including lucrative surgeries such as hip and knee replacements that both large and small hospitals rely on to balance their books.
The New Hampshire Hospital Association puts losses at more than $250 million in 2020.
At Elliot Hospital in Manchester, the recent decline in COVID-19 cases following the January spike has created openings for more of those elective procedures. Elliot’s president, Dr. Greg Baxter, said the hospital also didn’t suffer the same challenges in the recent spike of cases as it did last March, when a lack of supplies left medical facilities scrambling.
“First issue we had was PPE, right, when we had trouble getting that,” said Baxter. “So we’ve solved that one. And now the much hoped for vaccine is here, and that should place us in a position that we won’t have as much of a threat to our workforce and our ability to be ready.”
Along with keeping more people on the job, the vaccine is also a mental lift for health care workers, many of whom have now received both doses.
“The vaccination is sort of our ray of sunshine, our hope that the tables are going to turn in our favor,” said Barclay.