Since her son Gabe was 11 months old, Jessica Aviles’ life has been full of doctor's appointments. Gabe, now seven, has Duchenne muscular dystrophy, a condition that means all of his muscles will eventually break down, even his lungs and heart.
In the middle of a health care staffing shortage, people who could provide the at-home care Gabe needs are hard to find. After moving to New Hampshire to get better access to medical services, and to be closer to Gabe's longtime doctor in Massachusetts, Aviles is learning to provide at-home care herself.
She’s in training to become a licensed nursing assistant (LNA). Gabe qualifies for at-home care through New Hampshire’s Medicaid program. Eventually, she’ll be paid for her work.
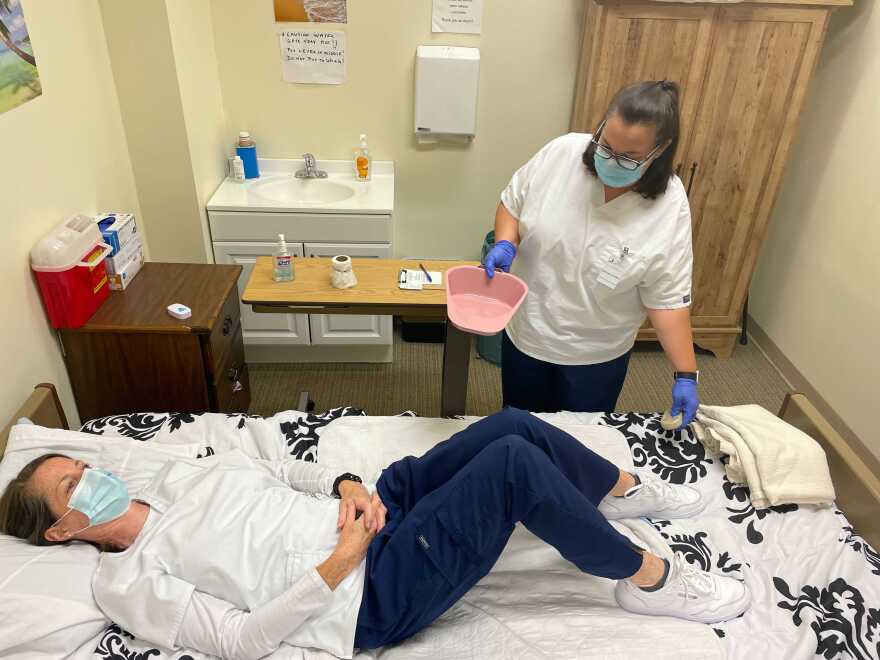
But first, she has to take a state exam to get her license. She trained for three weeks to get the certification, and lately, she’s been practicing her skills at a clinic in Manchester. She commutes there from her home in Campton.
At 46, she’s the oldest in her training cohort. The youngest is 19, and their group comes from New Hampshire and Vermont.

But working as an LNA is exhausting.
“I had no idea how much physical work this was,” Aviles says. She does everything from bed baths to changing briefs to procuring chocolate milk for residents.
For the past week, she’s been training full-time at a long-term care facility. At the end of the day, she goes home and does it all again with Gabe and her other children. While Gabe doesn’t need all the same types of care her clients at the long-term care center do, there’s a lot of overlap.
“I've been doing it all day and now I'm doing it at home for him,” Aviles says. And she also has to worry about the threat of COVID-19. Gabe is at risk and unable to get vaccinated, given his age.
She’s getting lots of emails from her daughter's high school about outbreaks in Campton. This week, there were 27 cases. But a new mask mandate at Gabe’s school is helping put Aviles’ mind at ease as she prepares for her next big step.
Brenda Rees, with LNA Health Careers, the LNA school Aviles attended, says she wishes more people did what Aviles is planning, but it’s possible not a lot of people know about the option.
If they did, she says, “they could still stay at home and care for their loved one.” And get paid to do it.
While wages in the industry are rising, they are still low, often starting at around $15-18 per hour says Rees. In the past month, both Solution Health, the parent company of Elliot Hospital, and Dartmouth Hitchcock Health have raised their minimum wage to $17 dollars an hour.
As employers compete for LNAs, hiring bonuses have climbed. Many facilities, Rees says, will also pay for a student's training at LNA Health Careers if the student will commit to working for them afterwards for a set amount of time.
Aviles paid the $2,000 for the course herself and she says it was a good investment. She now feels comfortable taking Gabe’s blood pressure and pulse. She won't immediately use all of the skills, she says, but some may prove useful later, as Gabe’s Duchenne's impacts his life more.
Even things that seem simple she says, like knowing how to shave his face or brush his teeth. “Once he loses that mobility, I’ll be able to go, I was trained for this, I know how to do this.
“Being able to meet more of his needs on a more professional level, I feel like it's going to make me a better mom to him,” Aviles said.
After NHPR reported this story, Aviles reached out. She passed her exam.
Once she gets her official license, she’ll be able to start work as an LNA. Her next step, she says, will be to find a home care agency that is willing to hire her as Gabe’s LNA.
Jessica Aviles is one of six women NHPR will follow as part of Overtime. And we want you to add your voice. How are you managing the needs of caregiving and work during the pandemic? What is changing for you as the pandemic fades?